More Perspectives on Low-Wage Workers in High Demand
Posted in Blog What's New
December 2021

$15 Minimum Wage Would Raise the Wage for One Third of the Home Health Aide Workforce by 2025, but the average worker would still earn below a Living Wage in nearly every state.
Carol B. Davis, PhD.
The Fight for $15 on behalf of Low-Wage Workers, includes Home Health Aides
Home Health Aides (HHAs) are often cited as low-wage workers whose fortunes motivate the push to raise the Federal Minimum Wage. For this blog post we explored the direct impact on HHAs of raising minimum wages according to the schedule in the most recent RTW bill, estimating that 32% of current HHAs would benefit directly by 2025.
The Raise The Wage (RTW) Act of 2021 proposal included incremental increases in the federal minimum wage starting at $9.50 for 2021, reaching $15 by 2025. Thereafter, growth in the federal minimum would be indexed to median income growth rates. Rep. Bobby Scott (D-VA), and Senator Bernie Sanders (I-VT) have introduced Federal Minimum Wage legislation unsuccessfully in each Congress since 2017. In 2021, the Bill was again reintroduced, and again, failed to garner enough support for consideration and successful passage in Congress to make it to the President’s desk.
How Many HHAs would benefit directly from the Federal RTW Schedule?
Our analysis considered the RTW 2021 schedule, comparing the annual hourly wage targets to a projected wage distribution for HHAs. We projected HHA wages using a uniform annual inflation rate of 2.8%, a level in the middle of long-term inflation projections from the Conference Board and the Congressional Budget Office. We applied that same inflation rate to current state level living wage estimates from the MIT Living Wage Calculator to compare the projected wage and potential wage under RTW with a practical anti-poverty threshold.
32% of current HHAs would benefit directly by 2025
We estimated that 13% of HHAs are in the 5 states where at least 25% of home health aides would likely have been due an increase as a direct result of the RTW schedule in 2021, making the RTW schedule a potential immediate benefit to approximately 102,400 HHAs, 3% of the U.S. HHA workforce.
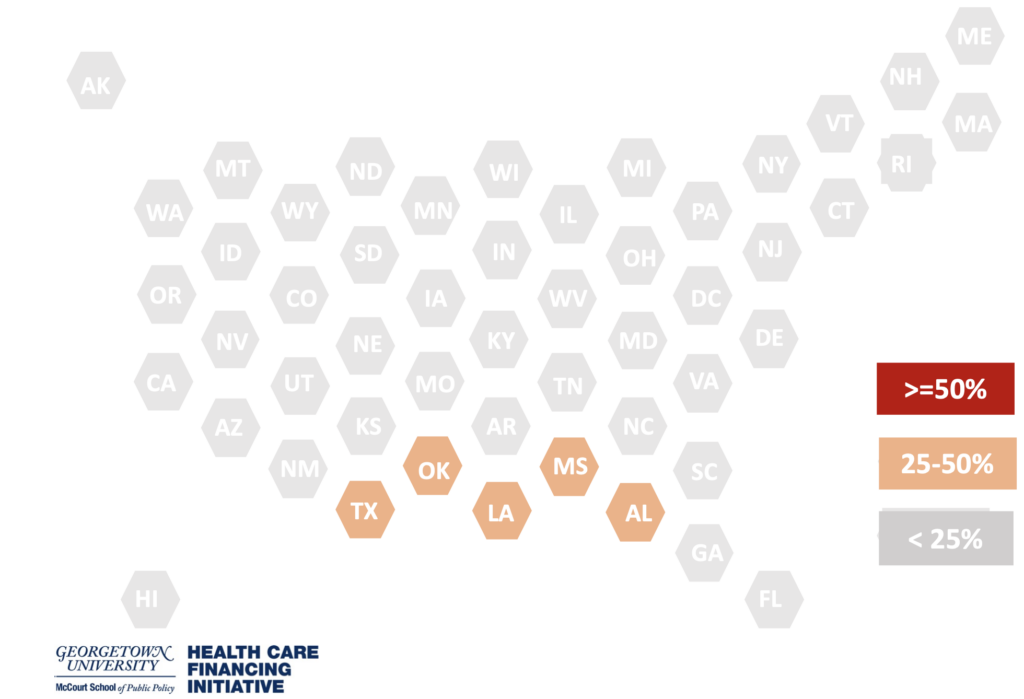
Figure 1: HOME HEALTH AIDES DIRECTLY BENEFITTING FROM FIRST YEAR OF RTW SCHEDULE
By 2025, the impact would be more widespread. We estimate 32% of the current HHAs, approximately 1,013,000 would benefit directly from the $15 minimum wage law as scheduled by RTW. Forty-seven percent of the current HHAs are in the 30 states (shown in red in Figure 2) where half of the workforce would benefit from the increased minimum wage law. The impact would expand to 44 states with at least 25% of the current HHA workforce gaining wages due to the Raise the Wage (RTW) Schedule. See Figure 2 or Figure 2 detail.
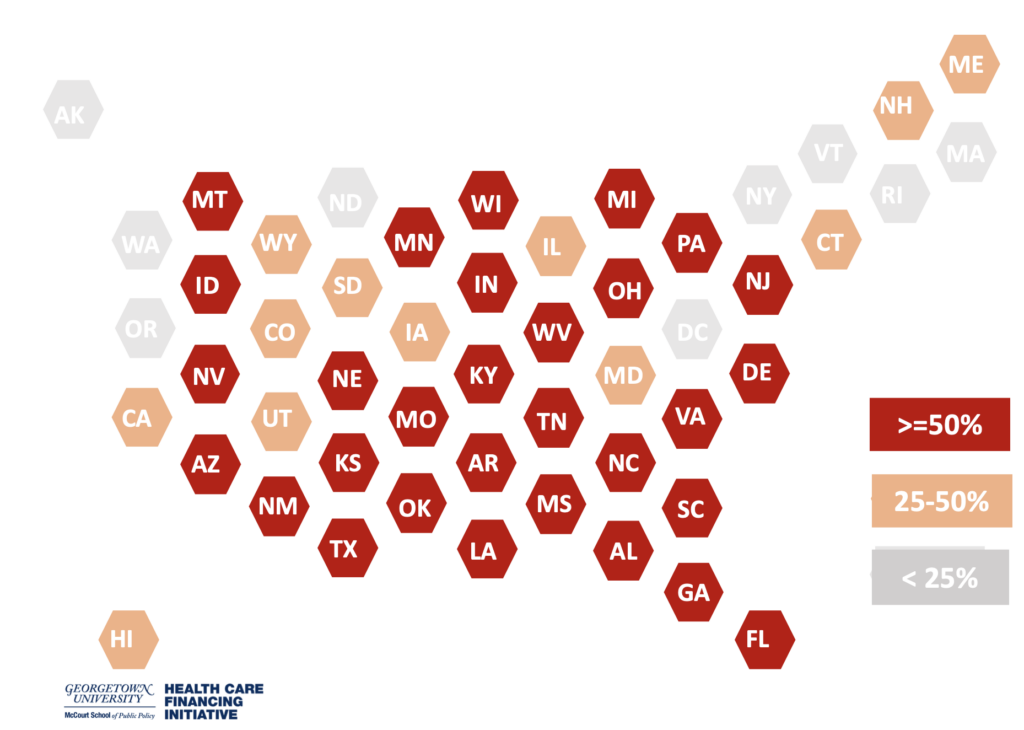
Figure 2: HOME HEALTH AIDES DIRECTLY BENEFITTING FROM RTW SCHEDULE by 2025
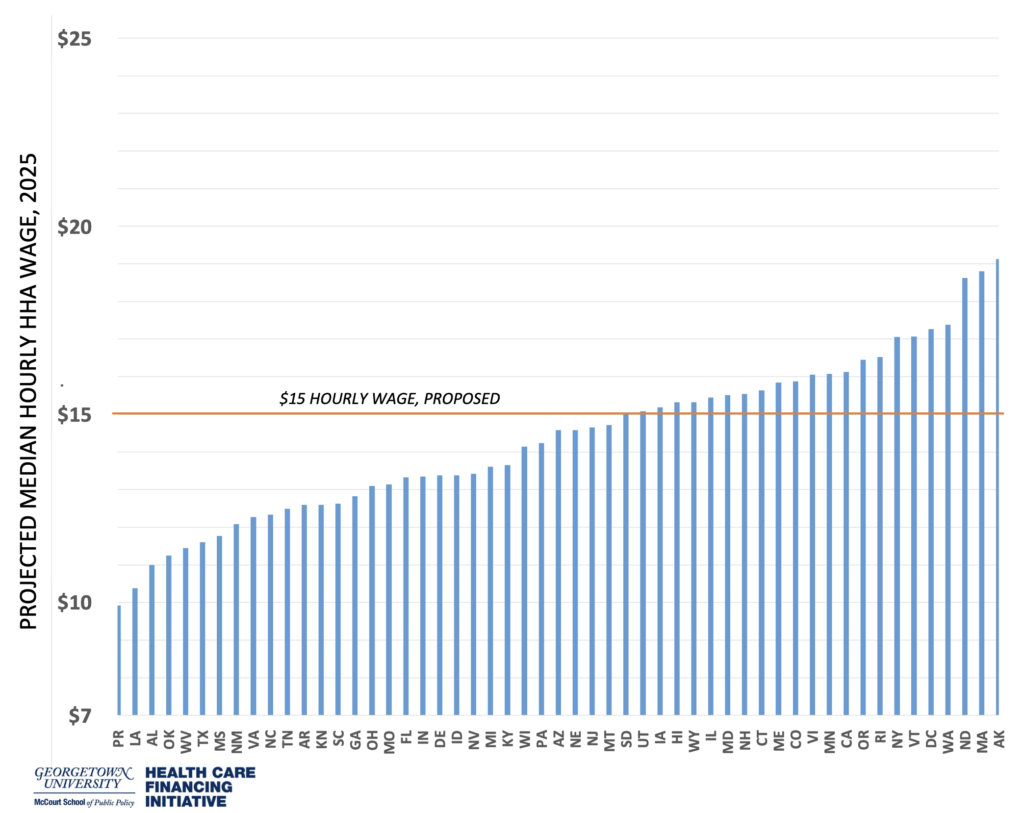
Figure 3: PROJECTED MEDIAN HOURLY WAGE, 2025 VS. $15 PROPOSED FEDERAL MINIMUM
Despite the obstacles at the federal level, individual states have made progress. Twenty-four states implemented minimum wage increases for 2021, though only a handful have mandated a $15 minimum by 2025. In 2022, social spending proposals are likely to remain highly contested, with the fortunes of essential workers at stake. Increased wages for HHAs might best be considered as a component of a suite of reforms that could address multiple objectives related to equitably growing and stabilizing the Home Care workforce for the benefit of both workers and the communities they serve.
Broader Agenda Needed to Stabilize and Secure an Essential HHA Workforce
Living Wage for Essential Workers
Our analysis suggests that the RTW schedule would improve wages for approximately one third of home health aides, raising wages more than 30% in the locations with the lowest wages as of 2021. However, in nearly every state, the median wage earning Home Health Aide would likely still earn less than a Living Wage for their state. the prospects for improving living standards for these essential, direct care workers across the nation is less compelling. For the median HHA in nearly every state, $15/hour would fall short of current projections for the median HHA wage and fall short of the Living Wage. If we compare the RTW $15 to projected Living Wage for 2025, the need for a more ambitious policy goal, to help attract and retain the essential direct care workforce, becomes clear. See Figure 4.
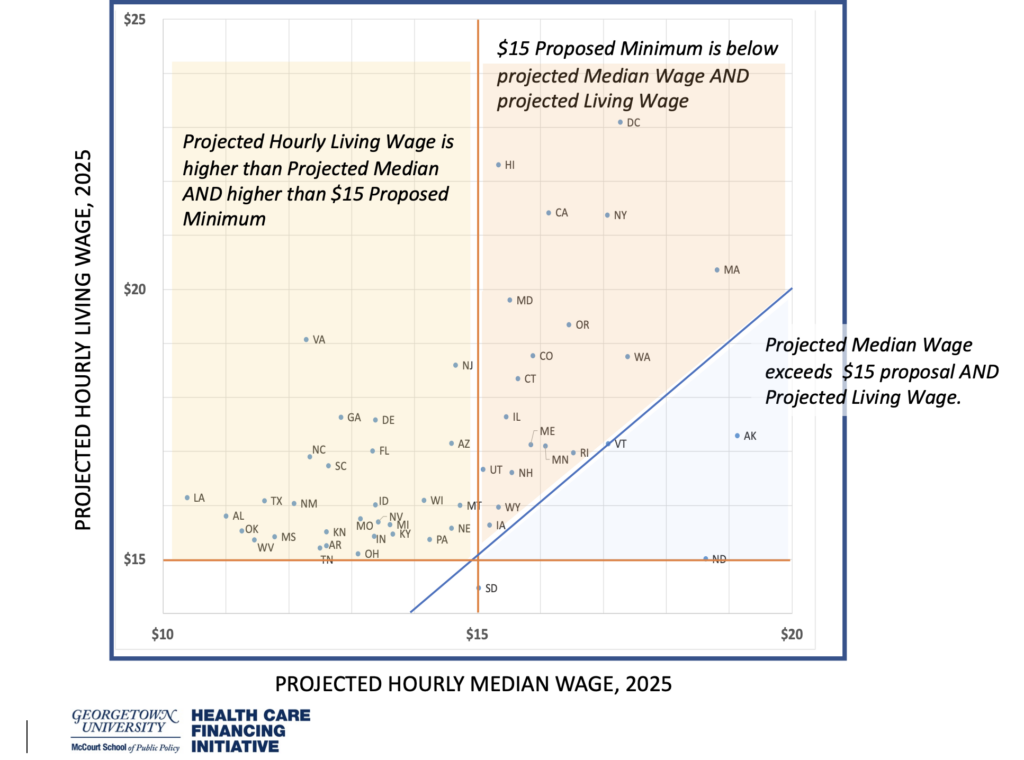
Figure 4: PROJECTED HOURLY MEDIAN WAGE VS. PROJECTED HOURLY LIVING WAGE, 2025
Growth and Stability of Essential, Direct Care Workforce
If we evaluate minimum wage legislation as a tool towards a broader policy objective: to grow and stabilize essential, direct care occupations, and ensure that services such as home-based care are broadly available as demand continues to grow over the next 10 years. The health care press has been reporting regularly this year about patients waiting weeks or months to get home care recommended by their physicians, due, in part, to record vacancies and job turnover in home care. Low wages are likely only a part of this instability. Policymakers bent on access for patients and stability for the direct care workforce ought consider a broader policy agenda for the next iteration of RTW legislation.
Equitable Returns to Work
Another significant , if indirect, result of RTW could be ensuring that increases in home health care agency productivity and revenues to go towards direct care worker wages. In its dual roles as payor and regulator, the federal government has the ability to use RTW in tandem with health care reimbursement policies and reimbursement schedules in such a way to ensure that home care providers have the additional funds to pay HHAs, and that the wage increases are targeted towards these currently low-wage direct care workers.
Equitable Access to Home-Based Health Care
The increased cost of HHA wages would be borne by a combination of reallocation within provider agencies, and price increases passed on to customers. Given the importance of Medicare and Medicaid in paying for home-based care (66% in 2020), more expansive benefit coverage and reimbursement terms could ensure that the burden of cost increases does not fall disproportionately on lower income patients or worse, preclude beneficiaries from receiving the in-home care they and their doctors choose.
It remains to be seen whether the national desire to emerge from the COVID-19 pandemic with a functioning, well-resourced health care infrastructure will lead government and market forces to prioritize wages and working conditions for HHAs and related occupations. If turnover rates and the Great Resignation is any indication, the workers are expecting more.
Dr. Carol Davis thanks the HCFI team for support of the analysis in this post. Research Assistant, Vidhur Krishna researched and analyzed state minimum wage and living wage calculations. Dr. Tom DeLeire provided valuable feedback on the analysis and the determination of inflation modeling assumptions. This extends analysis from our previous post by Analyst Teneil Brown profiling the current HHA Workforce.
References:
U.S. Department of Labor, Wage and Hour Division, https://www.dol.gov/agencies/whd/minimum-wage/state#wdc
Bureau of Labor Statistics, U.S. Department of Labor, Occupational Outlook Handbook, Home Health and Personal Care Aides,
at https://www.bls.gov/ooh/healthcare/home-health-aides-and-personal-care-aides.htm
Conference Board. https://www.conference-board.org/press/why-wages-are-growing-rapidly
Congressional Budget Office. https://www.cbo.gov/about/products/budget-economic-data#4
Massachusetts Institute of Technology, Living Wage Calculator: https://livingwage.mit.edu/
Centers for Medicare & Medicaid Services, Office of the Actuary, National Health Statistics Group. National Health Expenditures, 2020. https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/NationalHealthAccountsHistorical
National Conference of State Legislatures, ncsl.org/research/abor-and-employment/state-minimum-wage-chart.aspx